Shoulder Injuries: Dislocations versus Separations
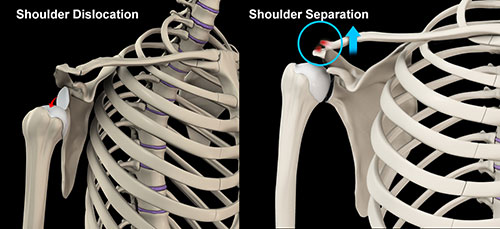
In the young athlete, shoulder injuries can be quite serious. Injuries can run the gambit, from simple strains (an injury to a muscle or tendon), sprains (an injury to a ligament), separations ( an injury to the acromioclavicular joint), dislocations ( an injury to the ball-in-socket, or glenohumeral joint), or fractures (broken bones). In this article I will clarify the shoulder separation and dislocation injuries, as these two often get mixed up.
A "separation" occurs when an athlete falls directly on the tip of the shoulder, with the arm against the side of the body. The joint that gets injured is actually the second joint about the shoulder area, the acromioclavicular joint. This is a relatively non-mobile joint formed between the end of the collar bone (clavicle) and the scapula (acromion process). Joint capsular ligaments as well as accessory ligaments, the coracoclavicular ligament which is divided into the conoid and trapezoid bundles, maintain the stability of this joint. With a "separation" some combination of these ligaments is injured, resulting in increased mobility of the clavicle in relation to the acromion. These injuries are typically graded I through III. In grade I injuries, the superior capsular ligaments are injured or torn, but the more stout remaining ligaments maintain good joint stability. The sign of the injury is usually localized swelling at the end of the collar bone and tenderness. In grade II injuries, more capsular ligaments are injured above and below the joint, and a partial injury to the coracoclavicular ligaments can occur, resulting in some instability at the joint and a slightly more prominent end of the collar bone. In grade III injuries, all of the ligamentous structures are torn, resulting in a frankly unstable joint and an obviously high riding collar bone.
A "dislocation" typically occurs when an athlete gets the arm forcibly stretched beyond its anatomical limits to the side of the body and rotated behing the head. The result is that the ball pops out of the socket. In some cases the ball may pop right back in the socket, but in many cases the ball gets stuck out of the socket, resulting in severe pain and an inability to move the arm. In the young athlete, to accomplish this, 80% of the time, a ligament in the front of the shoulder tears. The anterior-inferior glenohumeral ligament tears a portion of the cartilage ring, the labrum, from the socket (glenoid). The injury to the ligament and labrum usually does not heal perfectly on its own, resulting in long-term instability of the shoulder, with the potential for recurrent "dislocations".
The treatment for "separations" is quite different than for "dislocations". In "separations", the injury rarely requires a trip to the emergency room. Grades I and II are treated symptomatically, with a sling for comfort for a few days and restricted activities for a while. Grade III injuries are more difficult because of the obvious deformity created, but the current orthopedic literature and research continues to recommend a non-operative approach to this injury. Some surgeons have preferred surgical fixation of the injury, with mixed results. In "dislocations", the athlete usually has to go to the emergency room, unless the ball pops back into socket on its own. Popping the shoulder back into socket usually requires pain medicine, and/or an anesthesia, with a couple of strong helpers. After "relocation", the pain in the shoulder subsides promptly, and it can move and feel relatively normal within days. Unfortunately, with the probable torn ligaments, re-dislocation can occur easily if the arm is put in the wrong position. Signs of recurrent instability, such as re-dislocation, numbness and tingling down the arm, and pain, often will result in surgery to restabilize the joint, or repair the ligament.
These are very complex injuries, that are often confused for each other. The differences are substantial, and I hope this cursory review of the injuries helps athletes to understand them better. Both injuries should be evaluated by a Sports specialist, for appropriate treatment direction.